Retinoblastoma (RB)
Overview
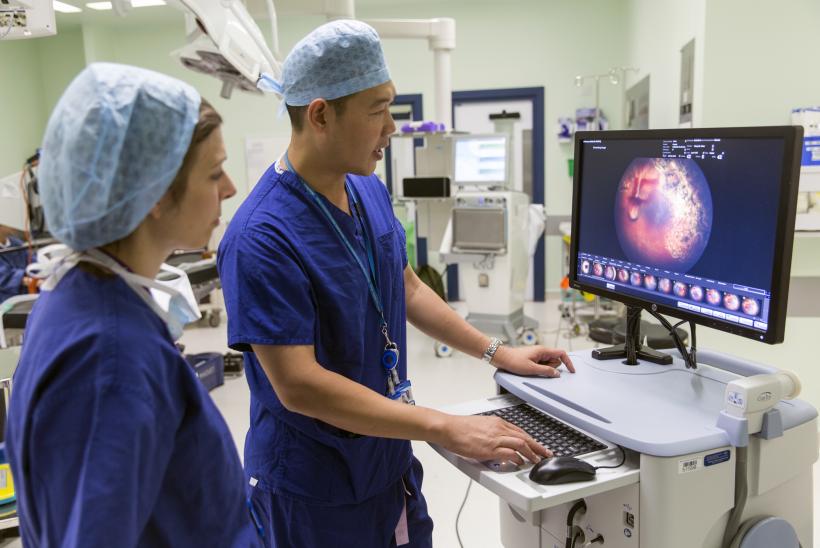
Retinoblastoma, also called ‘Eye Cancer’ is the commonest primary ocular malignancy of childhood, with tumours arising from the developing retina. Retinoblastoma is a malignant transformation of primitive retinal cells. Retinoblastoma accounts for up to 3 % of all tumours in infancy. This usually occurs before the age of 5 years. The incidence of sporadic retinoblastoma is 1 in 20,000 live births, with no gender or racial predilection.
RB Treatment at GOSH
Great Ormond Street Hospital for Children (GOSH) is a globally renowned children’s hospital, championing innovation across more than 60 clinical specialties and providing ground-breaking treatments for the rarest and most complex conditions. GOSH is one of the three largest centres for children with cancer/leukaemia in the western world and the largest in Europe.
The Haematology and Oncology department at GOSH is uniquely set up to treat the rarest and most complex forms of paediatric cancer. The service treats approximately 450 patients each year, accounting for about 28% of national childhood cancer cases.
Currently, the 5-year survival rate of RB is 99% and the 20-year survival rate is 85% in the UK. GOSH is one of only two treatment centres in the UK dedicated to treating retinoblastoma, and one of the largest centres for retinoblastoma in Europe. GOSH see 1/3rd bilateral and 2/3rd unilateral cases, in both genetic and non-genetic forms.
1/3 cases of retinoblastoma carry the genetic change and could be passed on to the next generation. The median age of presentation is 8 months. These cases also carry a lifelong risk of second cancers and always affect both eyes with poor vision. Moreover, 2/3 cases of retinoblastoma are sporadic/unilateral and the median age of presentation is 28 months. When only one eye is involved, a white reflex on photographs or squint is the commonest reason for referral.
Careful screening of the fellow eye is essential in all such cases through childhood. Screening of high-risk infants from 2 weeks of age- continues until at least 5 years. Early diagnosis and prompt treatment are therefore crucial to saving life and vision.
The aims of GOSH’s treatment Strategy are:
-
Preserve Life
-
Preserve vision/cosmesis
-
Minimise late effects (10% chance of the second tumour at 20 years)
A multi-specialist team
Cross-speciality expertise is key to delivering world-leading retinoblastoma treatments. At GOSH, expert teams from oncology, opthalmology and neuro-radiology will discuss each patient and agree the best individual treatment for that patient. A broader team including clinical nurse specialists and play specialists will ensure the patient and their family are fully aware of the treatment pathway and that a holistic approach is taken when providing the care.
Ongoing aftercare includes support from a range of professionals including psychologists and clinical geneticists. Our orthoptists assess vision and visual fields and provide support for schooling and information regarding maximising the child’s potential on the background of their visual impairment.
Treatment Options
- Enucleation (removal of the eye)
- Systemic Chemotherapy JOE Carboplatin, Vincristine, Etoposide - PK-guided doses requiring an increase of dose in all patients less than 3 months; IVAD 2nd line
- Intra-vitreal Chemotherapy weekly direct injection under anaesthesia ( x3)
- Intra-arterial Chemotherapy( Melphalan and topotecan x3)
- Cryotherapy (freezing treatment)
- Laser (heating the tumour to damage the cells)
- Radioactive Plaque
- Radiotherapy (lens-sparing)
Primary treatment offered is systemic intravenous chemotherapy/JOE chemotherapy, administered by central lines inserted by interventional radiology. This is offered as the first line of treatment for most patients. It usually lasts 6 courses which are 3-4 weeks apart. Patients are assessed initially at diagnosis with examination under anaesthesia, ultrasound and occasionally MRI and or orbital CT. Parents will also have their eyes examined and the blood will be sent for germline mutations. If they commence chemotherapy they are reviewed after 2 courses to ensure an ongoing response. The frequency of screening depends on the risk to each individual child determined by the agreed protocol.
Local therapies including laser and cryotherapy are offered by the ophthalmology team and administered under anaesthesia at the time of the examination. At relapse, we offer intravitreal chemotherapy, plaque radiotherapy and intra-arterial chemotherapy depending on the individual patient.
We are also able to offer a pharmokinetics dose modified service for delivering carboplatin chemotherapy in babies. This is important to minimise toxicity, in particular to their hearing (ototoxicity, nephrotoxicity) but also to ensure the efficacy of dosing. This is crucially important in the smaller babies who are often picked up on screening in the first weeks of life due to there being a positive family history.
Intra-arterial chemotherapy (IAC)
GOSH can provide intra-arterial chemotherapy (IAC), previously at the point of relapse but going forward as an upfront first line treatment for patients in group C and group D eyes. GOSH is the most experienced centre in the UK for IAC and can also offer VEPS (vision evoked potentials) to identify early visual loss during IAC treatment.
We can salvage eyes with IAC, and this is especially used for patients at relapse. This service is run with our specialised interventional neuroradiologists who are based at GOSH and Queens Square. Preservation of life is the most important management of our patients so we perform enucleations in collaboration with the world-leading artificial eye service at Moorfields Eye Hospital, which provides the support for the prosthetic eye.
During 2008 - 2017 GOSH treated 92 relapsed children (aged between 6 months – 12.5 years) with IAC. 63% of these cases were bilateral. Successful globe salvage rate was 59% with less than 1% morbidity and 1% permanent dysmotility.
GOSH has used intra-ophthalmic chemotherapy in 102 eyes in 92 children (GOSH 2008-2016):
- SIAC per eye 1-7 mean 3.1 (1 failed access)
- 43 boys, 42L 50R 10BL
- Mean age 3.2 year (6 months – 12.5 year)
- 63% bilateral (familial) disease
Enucleation
Enucleation is a life-changing procedure. 86% of unilateral children require an enuelation and a small percentage of bilateral children. The long team effects are not yet researched however a possible link to PTSS. Cosmetically can look good with a good range of movement and no pain when removed.
Summary of patients from 1st 2012 to the 31st December 2016:
- 73 unilateral + 45 bilateral eyes
- Enucleation rates (10 +20)
- Unilateral 53% and 7% of 73 eyes
- Bilateral 21% and 12% of 90 eyes
- (3 children had bilateral enucleations)
- 3 deaths (1 sepsis, 2 progression)
GOSH Outcomes 5-year Data
Between 2012-2016, GOSH treated 161 eyes, 73 unilateral and 88 bilateral, the majority grade D and E.
Unilateral outcomes:
Total patients n= 73; 53% of unilateral patients underwent primary enucleation of whom 38% received adjuvant chemotherapy for adverse histology. 47% of unilateral patients treated underwent JOE chemotherapy of which:
- Grade A 100% eyes preserved
- Grade B 100% eyes preserved
- Grade C 100% eyes preserved
- Grade D overall 88% eyes preserved but 100% of those in whom conservative (JOE chemotherapy) treatment was attempted
Bilateral outcomes:
45 patients 90 eyes- the eye salvage rate
- Grade A eyes 100%
- Grade B eyes 100%
- Grade C eyes 89%
- Grade D eyes 77% 100% of those given initial conservative treatment
- Grade E eyes 17% 34% of those given initial conservative treatment
Conditions we treat
- Retinoblastoma (RB)
Refer your child for treatment
Use the form below to refer your child for treatment. A member of our team will be in touch within 2 working days.
Mandatory fields